Why is my frozen shoulder so painful?
Frozen shoulder (adhesive capsulitis) is not just a stiff joint. It is a two-phase biological process that explains the extreme pain:
The two-phase problem
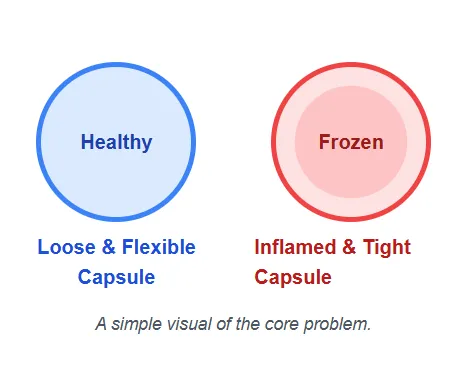
- Phase 1: Inflammation (“fire”): The joint capsule’s lining becomes inflamed (proliferative synovitis). This drives the deep, constant ache—especially at night.
- Phase 2: Fibrosis (“scar”): Activated fibroblasts lay down disorganized scar tissue, thickening and tightening the capsule. This shrinks joint volume and blocks motion.
Chemical “foremen” driving the process
- TGF-β: Signals fibroblasts to keep building scar tissue.
- IL-17A: Drives both inflammation and fibrosis.
What are the severe symptoms of frozen shoulder?
Symptoms often start subtly, then become unmistakable. Key signs include:
- Deep, aching pain that worsens at night and disrupts sleep.
- Progressive loss of motion—difficulty reaching overhead, behind the back, or across the body.
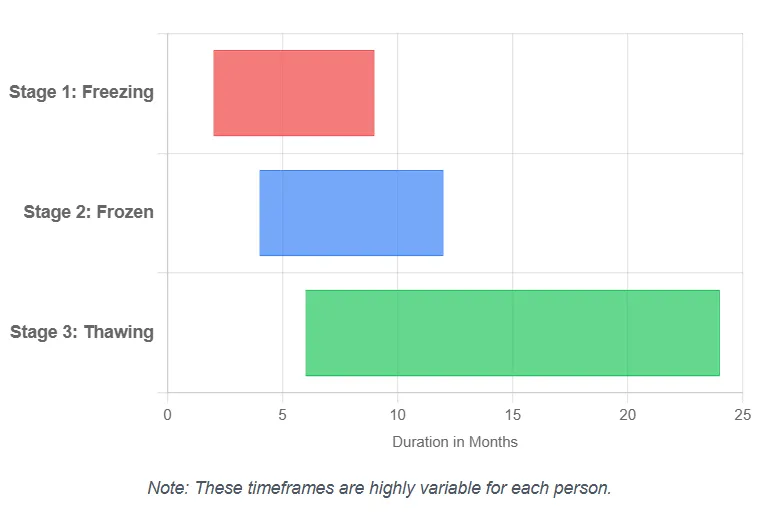
- Stage-dependent pattern: painful “freezing” stage → stiff “frozen” stage → gradual “thawing.”
- Daily-life impact: dressing, personal care, and reaching become difficult.

How do you ease the pain of a frozen shoulder?
Match relief to the disease stage. The goal is to calm inflammation, preserve comfortable motion, and protect sleep.
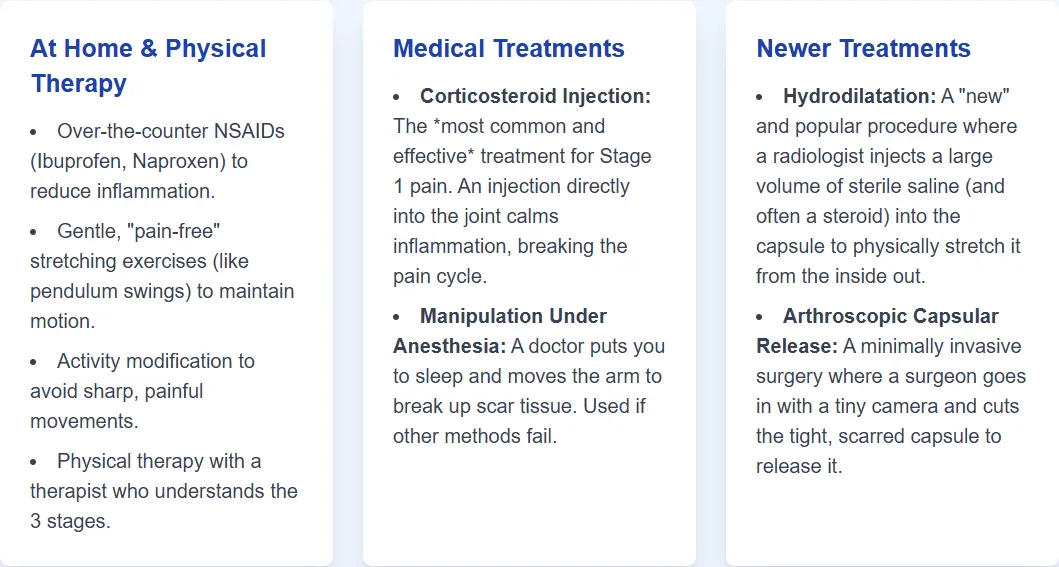
- Medication & modalities: NSAIDs, strategic heat/cold, and pillow positioning; many patients sleep better in a recliner early on.
- Early corticosteroid injection: Most effective in the pain-predominant stage (early Stage 2) to “cool the fire” and open a window for gentle motion.
- Gentle motion only during severe pain: Pendulum swings and pain-free range to avoid provoking inflammation.
- Guided physical therapy: Appropriate in the frozen and thawing stages to regain motion; aggressive stretching too early can backfire.
- Suprascapular nerve block: Option for refractory pain to improve sleep and tolerance for movement.
When to go to the ER for shoulder pain?
Frozen shoulder pain is severe but rarely an emergency. Seek immediate care for these red flags:
- Heart attack signs: Sudden chest discomfort with shoulder/arm pain, shortness of breath, cold sweat, nausea, or jaw/back pain (especially critical in women).
- Stroke signs (F.A.S.T.): Face drooping, Arm weakness, Speech difficulty—Time to call 911.
- Possible joint infection: Fever/chills, hot swollen shoulder, inability to move.
- Acute trauma: Obvious deformity after a fall or blow, severe sudden pain, inability to move, rapid swelling/bruising.

How long is the painful stage of a frozen shoulder?
Short answer
The painful “freezing” stage typically lasts 6 weeks to 9 months. Pain peaks early, then transitions to stiffness as the “frozen” stage begins.
Expect night pain and sleep disruption early. The next stage brings less pain but more stiffness. Early medical intervention—especially a steroid injection—may shorten the painful period.
Why does a frozen shoulder hurt so bad?
The pain is disproportionate because the tissue itself changes:
- Neoinnervation: New, sensitive nerve endings grow into the scarred capsule (linked to markers like nerve growth factor receptor p75), firing pain signals even at rest.
- Neoangiogenesis: New blood vessels form in the inflamed capsule, sustaining the inflammatory process.
- Central sensitization: Months of pain “turn up the volume” in the spinal cord and brain, so even light movement or clothing contact can feel extreme.
Bottom line: the capsule is biologically active, not just tight. Pain relief requires calming both the shoulder inflammation and the nervous system’s overreaction.
What is the new treatment for frozen shoulder?
“New” increasingly means combining proven tools to match the disease stage.
Emerging conservative options
- Corticosteroid injection + PT: Injection cools pain/inflammation; gentle PT restores motion. Often the highest-value pairing.
- Hydrodilatation: High-volume fluid (often with steroid) to expand the capsule. Evidence is mixed but low-risk.
- Suprascapular nerve block: Adds pain control to tolerate motion.
- Watchful waiting vs. formal PT: A 2024 AAOS study showed similar 1-year outcomes when both groups had access to corticosteroid injections, suggesting early pain control plus measured exercises may match intensive PT for some.
- Biologics under study: Platelet-rich plasma (PRP), hyaluronate injections, and future anti-fibrotic agents targeting TGF-β or IL-17A.
For refractory cases
- Manipulation under anesthesia (MUA): Surgeon carefully breaks adhesions while you’re asleep. Rare risks include fracture or nerve injury; less effective in insulin-dependent diabetes.
- Arthroscopic capsular release: Keyhole surgery to cut tight capsule bands. Provides rapid pain relief and motion gains; strong long-term outcomes.
Who is at risk & how to prevent it?
- Diabetes: Up to 20% lifetime risk due to glycosylation (“caramelizing” collagen). Early intervention and blood sugar control are critical.
- Thyroid disorders: Especially hypothyroidism.
- Age & sex: Most common between 40-60 and more frequent in women.
- Immobility after injury/surgery: Major preventable trigger—follow medical guidance for early, gentle motion after shoulder, breast, or chest procedures.
- Other associations: Parkinson’s disease and cardiovascular disease.
Think long game: frozen shoulder is a 1-3 year journey. The combination of staged pain control, gentle motion, and partnership with your medical team is the path to the thawing stage.