How do you get rid of frozen shoulder pain?
If you're reading this, your shoulder is likely in a state of painful, frustrating rebellion. Simple acts like reaching for a coffee mug, putting on a seatbelt, or just trying to sleep have become agonizing. You are not alone, and you are not imagining the severity of this pain. What you are likely experiencing is a condition called "frozen shoulder," or, in medical terms, adhesive capsulitis.
Getting "rid" of this pain involves understanding what it is, why it's happening, and then following a specific, science-based treatment path.
Understanding Your Pain: What Is Adhesive Capsulitis?
This isn't a simple muscle strain. The problem lies deep inside your shoulder, in the joint capsule. Your shoulder is a ball-and-socket joint, and this capsule is a strong, sac-like sleeve of connective tissue that encloses the joint, holding everything together.
In a healthy shoulder, this capsule is flexible and loose, allowing for a wide range of motion. It's also lubricated by a small amount of synovial fluid.
In a frozen shoulder, a process of inflammation and fibrosis (scarring) begins.
- The Capsule Inflames: The capsule becomes inflamed, thick, stiff, and tight.
- Adhesions Form: Thick bands of scar-like tissue, called adhesions, develop within the capsule, essentially "gluing" the joint together.
- Lubrication Decreases: To make matters worse, the amount of synovial fluid in the joint often decreases.
The result is a shoulder that is "stuck" or "frozen," leading to the two hallmark signs of the condition: severe, often-debilitating pain and a dramatic loss of movement.

The Two Types of Frozen Shoulder: Primary vs. Secondary
A critical first step in your diagnosis is figuring out why this happened. Frozen shoulder is broadly split into two types:
Primary (Idiopathic) Adhesive Capsulitis: This is the "mysterious" form. It occurs without any obvious injury or cause. The cause is unknown, but it's thought to be related to an underlying inflammatory or fibrotic process in your body. As we'll discuss, it is strongly linked to other systemic diseases.
Secondary Adhesive Capsulitis: This form is a result of a known event or condition. This is often broken down further:
- Intrinsic: Caused by a problem inside the shoulder, like a rotator cuff injury or tendinopathy.
- Extrinsic: Caused by a problem near the shoulder, such as surgery on the chest wall or breast, or a problem in your neck (cervical disk disease).
- Systemic: Caused by a whole-body disease.
Population Focus: Who Is Most at Risk?
This condition does not strike randomly. There are very clear risk factors, and seeing if you fit this profile can be a key part of the diagnosis.
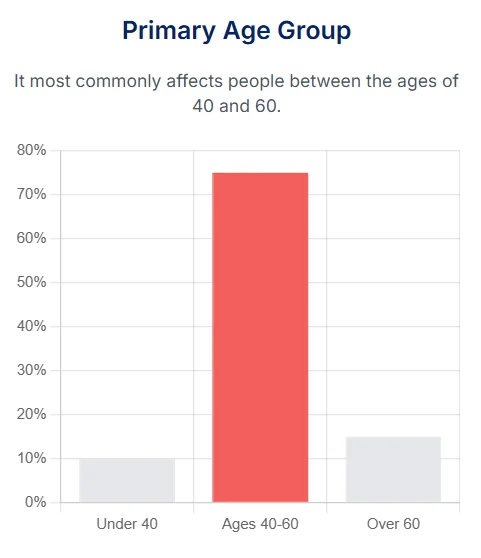
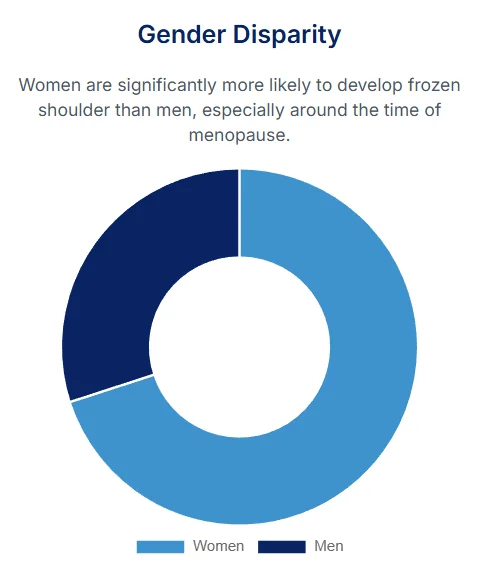
Age and Sex: Frozen shoulder most commonly affects people between the ages of 40 and 60. It is also significantly more common in women. We will explore this link to menopause in-depth in a later section.
Immobility (The Preventable Cause): This is the single biggest driver of secondary frozen shoulder. Any event that forces you to keep your shoulder still for a long time (immobilization) is a classic trigger. Common culprits include:
- Recovering from shoulder surgery
- Wearing a sling after a broken arm or a rotator cuff injury
- Recovering from a stroke, which can lead to lack of arm use
- Recovering from chest or breast surgery
Important Medical Connection
Systemic Diseases (The Big Three): This is perhaps the most important connection for primary frozen shoulder. Its appearance is a massive red flag to check for other, underlying conditions.
Diabetes: This is the most critical link. Frozen shoulder occurs "much more often" in people with diabetes. In fact, people with diabetes are up to 5 times more likely to develop it, and they account for nearly a third of all cases. The reason is thought to be a process called glycosylation, where excess sugar (glucose) molecules in your blood attach to the collagen in your joint capsule, making the tissue stiff, sticky, and prone to fibrotic "gumming up".
Thyroid Disorders: A strong, well-established link exists with both an underactive (hypothyroidism) and overactive (hyperthyroidism) thyroid.
Other Conditions: It's also associated with Parkinson's disease, autoimmune conditions, and cardiovascular disease.
The appearance of a "primary" frozen shoulder, especially in the 40-60 age range, should be a signal to you and your doctor to get a full blood panel to check for undiagnosed diabetes and thyroid dysfunction. It's often a "canary in the coal mine" for a systemic issue.
The Three (or Four) Stages: A Patient's Roadmap
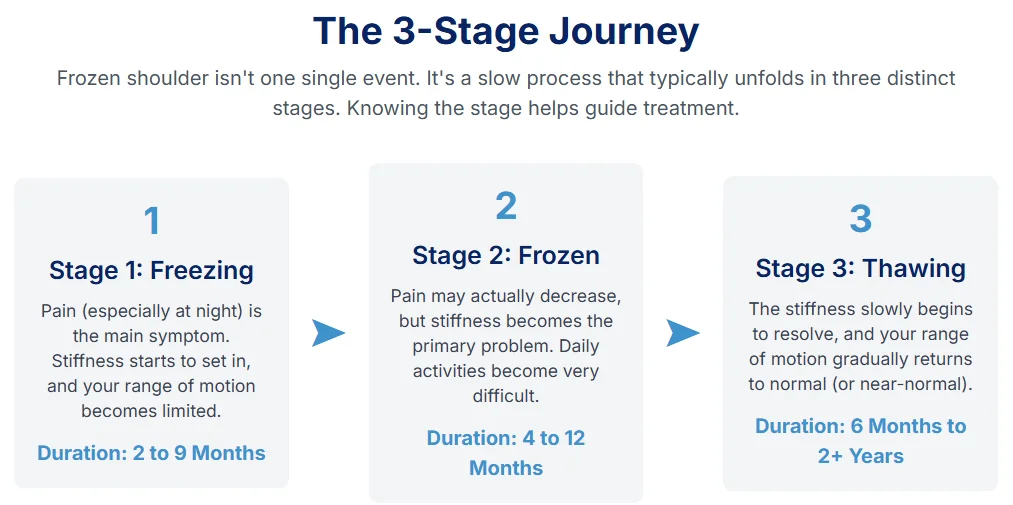
To understand the treatment, you must first understand the journey. Frozen shoulder isn't one single event; it's a slow process that is famously described in three (and sometimes four) stages.
| Stage | Also Known As | Typical Duration | What It Feels Like | Primary Treatment Goal |
|---|---|---|---|---|
| (Stage 0: Pre-Freezing) | (Pre-Adhesive) | N/A | Early aches, sharp pain at the end of your range of motion | Prevention (gentle motion) |
| Stage 1: Freezing | (Painful Phase) | 6 weeks – 9 months | Severe, deep, aching pain, especially at night. Stiffness begins, and you progressively lose motion | PAIN CONTROL (Steroid shot, NSAIDs, gentle motion) |
| Stage 2: Frozen | (Stiff/Adhesive Phase) | 4 – 12 months | Pain may lessen or subside. Stiffness dominates. Daily tasks become extremely difficult | RESTORE MOTION (Physiotherapy, stretching, hydrodilatation) |
| Stage 3: Thawing | (Recovery Phase) | 6 months – 2+ years | Stiffness slowly improves. Pain is minimal, but motion gradually returns | REGAIN STRENGTH & FULL FUNCTION (More advanced PT, strengthening) |
This roadmap is crucial because the treatment must be tailored to the stage you are in. What works for the "Frozen" stage can make the "Freezing" stage much worse.
The Treatment Ladder: A Step-by-Step Guide to Getting Rid of It
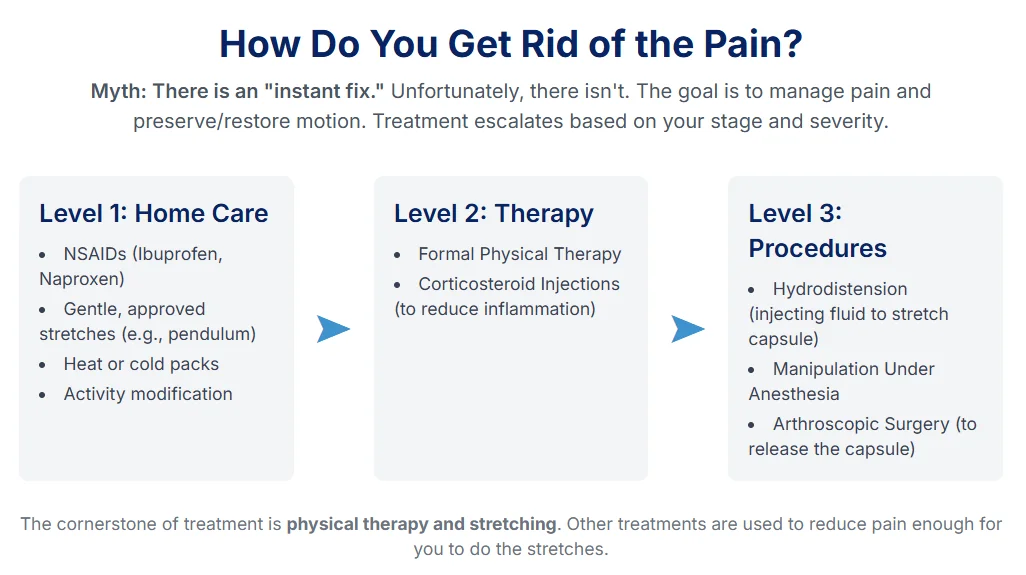
Treatment for frozen shoulder is best thought of as a ladder. You start on the first rung, and if that doesn't provide relief, you move to the next.
Step 1: First-Line Conservative Treatment (At Home and PT)
This is the foundation of recovery, focusing on pain control and restoring motion.
Pain Relief: The first step is to manage the pain and inflammation. Over-the-counter NSAIDs (nonsteroidal anti-inflammatory drugs) like ibuprofen (Advil, Motrin) or aspirin are the first choice because they do two jobs: reduce pain and calm the inflammation that's causing the problem. Acetaminophen (Tylenol) can help with pain but does not target inflammation.
Physiotherapy (PT): This is the cornerstone of treatment. A physical therapist will create a program of specific stretches and range-of-motion (ROM) exercises to gently "un-stick" the capsule. Common exercises include:
- Pendulum Swings: You lean over, let your affected arm hang down like a rope, and use your body to make small, gentle circles. This uses gravity to open the joint.
- Finger Wall Walks: You face a wall and "walk" the fingers of your affected hand up the wall, as high as you can comfortably go.
⚠️ CRITICAL CAVEAT: The "No Pain, No Gain" Myth
This is false. Your shoulder is in a state of high inflammation. If you try to "break through" the stiffness with aggressive, painful stretching, especially in the early "Freezing" stage, you will only increase the inflammation, anger the joint, and make the capsule thicken and stiffen more. The rule is: Stretch to the point of discomfort or a "good stretch," but NEVER to the point of sharp, searing, or agonizing pain.
Step 2: Medical Interventions (When Step 1 Isn't Enough)
If after several weeks of dedicated, gentle PT and NSAIDs, the pain is still unbearable, your doctor has powerful tools to help.
Corticosteroid Injections: This is often a game-changer. Your doctor injects a powerful anti-inflammatory medicine (a corticosteroid) directly into the shoulder joint.
Why it works: It's like a fire extinguisher, putting out the "fire" of inflammation inside the capsule. This can dramatically reduce pain, especially if given during the painful "Freezing" stage. The goal of the shot is to calm the shoulder down so that you can effectively participate in your physical therapy.
POPULATION CAVEAT (Diabetes): If you have diabetes, you must tell your doctor. A steroid injection can cause a temporary but significant spike in your blood sugar levels for several days. You will need to monitor your glucose very closely post-injection and may need to adjust your medication with your endocrinologist's guidance.
Hydrodilatation (or Hydrodistension): In this procedure, a doctor injects a large volume of sterile saline (water), often with a steroid, into the joint capsule. The goal is to use the hydraulic pressure of the fluid to physically stretch and "pop open" the tight, shrunken capsule from the inside.
Step 3: Surgical & Procedural Options (For "Refractory" Cases)
If 6-12 months of conservative treatment (PT, injections) have failed and you are still "frozen," these options may be considered.
Manipulation Under Anesthesia (MUA): You are put to sleep with general anesthesia. The surgeon then forces your shoulder through its full range of motion, which physically stretches or tears the tight capsule and adhesions.
Arthroscopic Capsular Release (ACR): This is a minimally-invasive "keyhole" surgery. A surgeon inserts a tiny camera and pencil-sized instruments into your shoulder and surgically cuts (releases) the thickened, tight, and fibrotic joint capsule.
Many surgeons now prefer ACR because it is a more controlled and precise procedure. MUA is "blind," and while effective, it carries small risks of accidentally causing a bone fracture or a rotator cuff tear. With ACR, the surgeon can see exactly what they are cutting, visually confirm the diagnosis, and even treat any other problems (like a biceps tendon issue) at the same time.
| Treatment | What It Is | Best For (Stage) | Pros | Cons / Key Risks |
|---|---|---|---|---|
| NSAIDs (Ibuprofen) | Over-the-counter anti-inflammatory | Freezing (Stage 1) | Good first-line pain/inflammation control | Can cause stomach upset. Does not "fix" the underlying stiffness |
| Physiotherapy (PT) | Guided stretching & ROM exercises | All stages (but different exercises per stage) | Essential for restoring motion | CAVEAT: Pushing too hard in Stage 1 can worsen pain and inflammation |
| Corticosteroid Injection | Steroid (anti-inflammatory) injected into the joint | Freezing (Stage 1) | Fastest way to reduce severe pain/inflammation. Enables effective PT | Temporary blood sugar spike in diabetics. "Cortisone flare" (transient pain). Rare risk of infection, tendon weakening |
| Hydrodilatation | Sterile fluid injected to physically stretch the capsule | Frozen (Stage 2) | Can physically stretch the tight capsule | Evidence is mixed; may not be better than a steroid injection alone |
| Manipulation Under Anesthesia (MUA) | Forcibly moving the shoulder while you are asleep | Refractory (Stage 2/3) | Non-surgical. Effectively breaks up adhesions | "Uncontrolled" procedure; small risk of fracture or rotator cuff tear |
| Arthroscopic Capsular Release (ACR) | Keyhole surgery to cut the tight capsule | Refractory (Stage 2/3) | Precise, controlled release. High success rate for restoring motion | It's surgery. Carries risks of anesthesia, infection. Requires diligent post-op PT |
RED FLAGS: When Your Shoulder Pain is NOT Frozen Shoulder
This is a critical safety check. Frozen shoulder is often a "diagnosis of exclusion," meaning your doctor must first rule out other, more serious conditions.
The hallmark sign of a true frozen shoulder is a significant loss of both active range of motion (you trying to move your arm) and passive range of motion (when a doctor tries to move your arm for you). The loss is especially profound in external rotation (turning your arm outward, like the "stop" signal).

⚠️ Seek URGENT medical help if you have any of the following:
- Acute Trauma: The pain started suddenly and intensely after a specific injury, like a fall or a car accident
- Systemic Symptoms: You have the shoulder pain plus a fever, chills, night sweats, or unexplained weight loss
- Significant Neurological Symptoms: You have profound weakness or numbness and tingling that radiates down your arm
- Visible Deformity: The shoulder joint looks visibly misshapen, or you have a large, localized swelling
How do I get instant relief from frozen shoulder?
This is the question everyone asks when they are in the depths of the "Freezing" stage, often in the middle of the night when the pain is at its worst.
Managing Expectations: The "Instant" Relief Myth
First, let's be honest about the word "instant." Because frozen shoulder is a chronic inflammatory and fibrotic process—where your joint capsule is physically thickening and scarring—there is no single "instant" cure that makes the condition disappear in 10 minutes.
The goal of "instant relief" is immediate pain management. It's about breaking the acute pain cycle, reducing inflammation, and, most importantly, getting some sleep.
At-Home Triage for Acute Pain
Here is your emergency action plan for when the pain flares up.
Medication: As mentioned before, NSAIDs (ibuprofen) are a go-to. They are better than acetaminophen (Tylenol) in this specific case because they target the inflammation that is the root cause of your acute pain.
Strategic Heat vs. Cold: These are not interchangeable. They have very different jobs.
- Use COLD (Ice Pack): Use a cold pack (wrapped in a thin towel to protect your skin) for 15-20 minutes to help "calm it down." Cold numbs the area, dulls pain signals, and can help reduce acute, sharp inflammation and swelling.
- Use HEAT (Heating Pad): Use a heating pad or a warm shower to help "loosen it up." Heat is excellent for relaxing the tight, stiff, and exhausted muscles around the shoulder joint. Many people find it's most effective to use heat for 15 minutes before doing their gentle exercises to make the tissues more pliable.
Gentle, Pain-Free Movement: When you're in pain, your instinct is to stop moving your arm entirely. Do not do this. Keeping it perfectly still will make it stiffer. You must find the "sweet spot" of gentle motion.
The Pendulum Swing: This is the #1 exercise for the acute, painful "Freezing" stage. Stand, bend over at the waist, and let your affected arm hang straight down. Relax your shoulder. Gently rock your body back and forth or in small circles, letting gravity and momentum swing your arm. Do not use your shoulder muscles to lift your arm. This movement is passive, and it uses gravity to gently create space in the joint without straining it.
Exercise Support: A shoulder pulley system can help you perform controlled, gentle range-of-motion exercises at home as part of your physical therapy routine, complementing the pendulum swing technique for gradual recovery.
The Night-Time Pain Problem: How to Sleep
The "worse at night" phenomenon is a defining and cruel feature of frozen shoulder. This happens for two main reasons:
- Mechanical Pressure: When you lie down, you are more likely to lie on the shoulder or have it collapse into a painful, compressed position.
- Physiological Changes: At night, your body's blood flow and inflammatory processes change. All inflammatory conditions tend to feel worse at night as inflammatory chemicals "pool" in the joint, increasing internal pressure and pain.
Poor sleep is not just a symptom—it's an aggravating factor. It lowers your pain tolerance, increases stress, and worsens systemic inflammation, creating a vicious cycle. Therefore, using pillow strategies is not "coddling" your shoulder; it is an active treatment to break this cycle.
Pillow Strategies for Pain-Free Sleep:
- If you sleep on your back: This is often the best position. Place a pillow under your knees to take pressure off your lower back. Then, place a thin pillow or folded towel under your affected arm (from the elbow down) to support it in a neutral, slightly elevated position. This stops it from "falling" to your side.
- If you sleep on your side: You must lie on your unaffected side. Do not sleep on your frozen shoulder. To protect the affected arm on top, hug a body pillow or place a thick pillow between your arms, tucking it high up into the armpit of the affected arm. This props the arm up and prevents it from collapsing forward and inward across your body. Placing a pillow between your knees also helps with spinal alignment.
- If you sleep on your front: We strongly advise against this. It's nearly impossible to find a position that doesn't twist your neck or put your shoulder in a compromised, painful position.
The Recliner Trick: Many, many people with frozen shoulder discover that the only way to get sleep during the "Freezing" stage is in a recliner. This semi-upright position keeps the joint in a neutral, low-pressure state. There is no shame in this; do what you must to get rest.
The Closest Thing to "Instant" Medical Relief: An Injection
If these at-home measures are not cutting it, the fastest medical intervention to get relief is a corticosteroid injection. As described in the previous section, this shot delivers a powerful anti-inflammatory directly to the source of the fire.
While the anti-inflammatory effect takes a few days to build, many injections also include an anesthetic (numbing medicine) to provide some pain relief right away. Be aware of the common side effects:
- "Cortisone Flare": It is common for the pain to get worse for the first 24-48 hours after the shot, as the steroid crystalizes and irritates the joint. This is normal and will pass.
- Other Side Effects: Temporary facial flushing, a "wired" feeling or insomnia, and (for diabetics) a blood sugar spike are all common.
- Rare Risks: Though rare, risks include infection, nerve damage, tendon weakening, and skin thinning (atrophy) or lightening (hypopigmentation) at the injection site.
An injection is not a "cure," but it can be an incredibly effective bridge. It can dial the pain down from a 10 to a 4, allowing you to finally sleep and—most importantly—begin the physiotherapy that is essential for your long-term recovery.
Does frozen shoulder pain ever go away?
This is the question that weighs on everyone's mind, especially after months of pain. You feel "stuck" and are terrified this is your new normal.
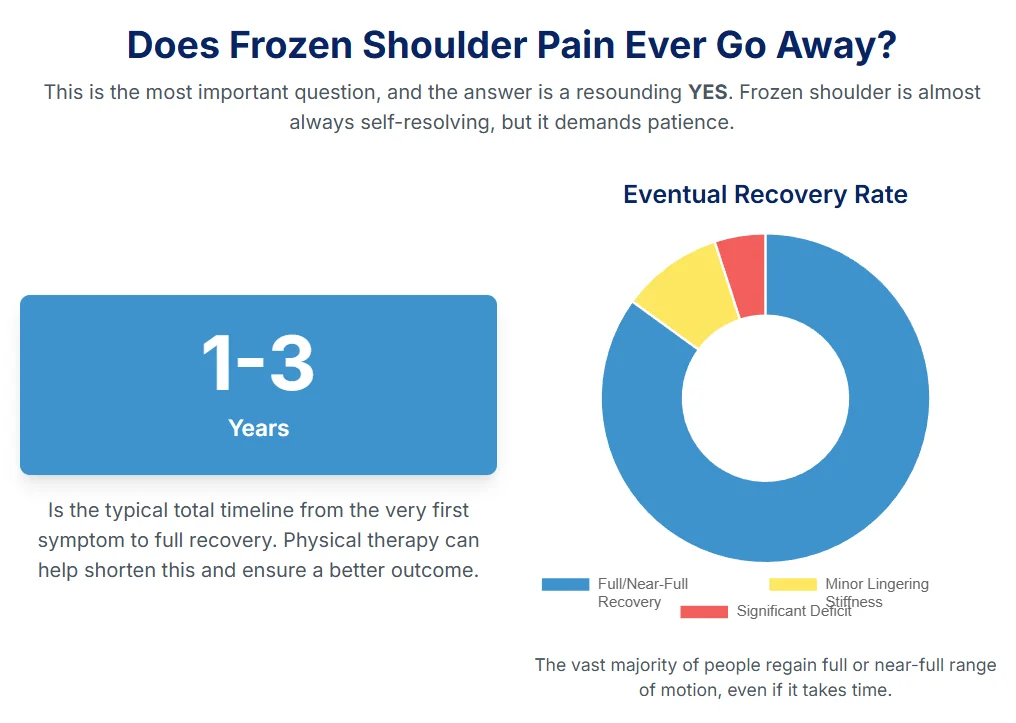
Let's start with the reassuring (but incomplete) answer you'll find on most websites: Yes, for the vast majority of people, the severe pain and stiffness of frozen shoulder does go away.
The commonly cited timeline for this "natural history" is 1 to 3 years. The condition is supposed to progress through its stages (Freezing, Frozen, Thawing) and then resolve on its own.
MYTH VS. FACT: The "It Always Resolves 100%" Myth
Now, let's get to the science-based reality. This is one of the biggest myths in musculoskeletal medicine.
The Myth: For decades, it was widely believed and taught that frozen shoulder is a "self-limiting" condition that always resolves to 100% normal function, even if you do nothing.
The Origin of the Myth: This idea can be traced back to a single, methodologically flawed study by Brian Reeves in 1975. This study had major issues, including causing stiffness in patients by putting their arms in immobilizing slings for 10-36 weeks, and then labeling their slow recovery from that immobilization as the "natural history" of the disease.
The Scientific Fact: In 2017, a landmark systematic review titled "Natural history of frozen shoulder: fact or fiction?" analyzed all the available evidence and found NO evidence to support the idea that frozen shoulder progresses through recovery phases to full resolution without treatment.
The Reality of "Recovery": What to Expect
So what really happens?
While the debilitating, 10/10 pain almost always resolves, a significant number of people (studies estimate between 20% and 50%) may be left with persistent, long-term symptoms, most commonly a mild loss of motion.
One long-term study that followed patients for an average of 4.4 years found that 41% of patients still reported some ongoing symptoms. But here is the crucial caveat: for the vast majority of those (94%), the remaining symptoms were mild and not functionally limiting. Only 6% of the total group had severe, long-term pain and functional loss.
So, Why Bother With Treatment?
This is the logical follow-up. If the myth is false, does treatment even matter? YES. Emphatically.
This new understanding fundamentally changes the purpose of treatment.
Treatment Goals:
- To Shorten the Timeline: To help you recover in 6-9 months instead of 2-3 years
- To Reduce Suffering: To manage the severe pain of the "Freezing" stage
- To Maximize Your Final Outcome: To aim for full 100% recovery, rather than being one of the 41% who settles for a "mild" but permanent loss of motion
Population Focus: Prognosis Is Not the Same for Everyone
Your long-term outlook is also heavily influenced by your overall health. The prognosis is generally less favorable for certain groups:
- Diabetic Patients: The evidence suggests people with diabetes tend to have a worse prognosis. The course of the disease is often longer, more severe, and more resistant to all forms of treatment.
- Thyroid Patients: This group may also experience a longer and more severe course.
- Severity at Onset: A key finding from one study is that patients who had the most severe symptoms at the beginning of the condition had the worst long-term prognosis.
This last point is incredibly important. It suggests that aggressively treating the pain and inflammation in the early "Freezing" stage (for example, with an early steroid injection) isn't just for your comfort—it might actually be prognostic. By "putting out the fire" early and preventing you from having those "most severe symptoms," we might be improving your long-term chances of a full recovery.
How do you treat a frozen shoulder in menopause?
This is an incredibly specific and insightful question. If you are a woman in your 40s or 50s and you've developed a frozen shoulder "out of nowhere," you are not imagining the connection. This is not a coincidence.
The Hormonal Connection: Why Menopause is a Risk Factor
Women in the perimenopausal and postmenopausal age range (typically 40-60) are the absolute primary demographic affected by "primary" (idiopathic) frozen shoulder.
For years, this link was considered coincidental, but modern research is building a strong case for a direct hormonal connection.
- Estrogen's Protective Role: Your joint capsules, tendons, and muscles have estrogen receptors. Estrogen plays a vital, protective role in your musculoskeletal system: it helps maintain the integrity and elasticity of connective tissues, stimulates muscle repair, and helps reduce inflammation.
- The Estrogen Drop: During perimenopause and menopause, your estrogen levels begin to fall, sometimes dramatically.
- The Result: This loss of estrogen is thought to create a "perfect storm" in the shoulder capsule. The tissue may become less elastic, tendons less flexible, and your body's baseline level of inflammation may increase.
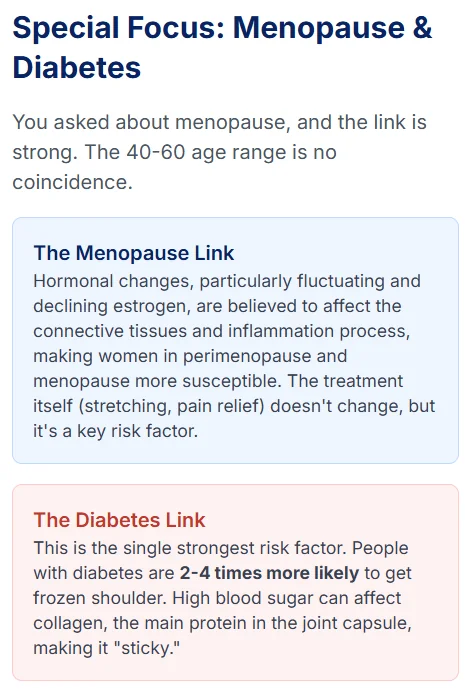
Emerging Research: Can Hormone Therapy (HRT) Help?
This is the cutting edge of the research. A 2022 study from Duke University researchers, presented at the North American Menopause Society (NAMS) meeting, investigated this very link.
The study analyzed nearly 2,000 post-menopausal women and found that those not receiving hormone therapy had greater odds of developing adhesive capsulitis.
The implication is that Hormone Replacement Therapy (HRT) may be protective against developing frozen shoulder in the first place.
Crucial Caveat: This research is new. HRT is not currently a standard "treatment" for an existing case of frozen shoulder. However, if you are in this demographic and suffering from frozen shoulder (or other new-onset joint pains and stiffness), it is a vital topic to discuss with your primary care provider or gynecologist.
Is the Treatment Any Different?
This is the key question, and the answer is "No" and "Yes."
No: The "gold standard" orthopedic treatments are exactly the same. The treatment ladder still applies:
- Pain Relief: NSAIDs, heat/ice
- Physiotherapy: Gentle, progressive range-of-motion exercises
- Injections: Corticosteroid injections are still a primary and effective tool
- Surgery: Arthroscopic capsular release is the same procedure for refractory cases
Yes: The context and holistic approach should be completely different.
Treating a frozen shoulder in a menopausal woman as just an "isolated shoulder problem" is a missed opportunity. A good treatment plan must be holistic and address the systemic and psychosocial factors at play.
Holistic Treatment Approach:
- Hormone Consultation: Your treatment should include a consultation with your primary care provider or a menopause specialist to discuss your hormonal status and the risks/benefits of HRT for your overall joint, bone, and cardiovascular health.
- The Thyroid Connection (Again): This is the other major endocrine disorder that peaks in women in this age group. Thyroid disorders can increase your risk of frozen shoulder by 2.69 times. The onset of frozen shoulder should be an automatic trigger for your doctor to run a full blood panel checking not only your blood sugar (for diabetes) but also your thyroid function (TSH).
- Psychosocial Stress: This is a major, overlooked factor. Women in this age group are often in a period of extreme stress from managing teenage children, caring for elderly parents, high career demands, and marital difficulties. This chronic stress leads to high cortisol levels, which dysregulates the immune system and increases systemic inflammation.
Therefore, any treatment plan that doesn't also include stress management and sleep hygiene is only treating half the problem.
What aggravates a frozen shoulder?
This is one of the most important things to learn. Managing a frozen shoulder is as much about what not to do as it is about what to do. The central challenge of this condition is a "tightrope walk": you must move it to get better, but moving it hurts, and moving it the wrong way makes it worse.
Here is your "Do Not Do" list:
Activities That Worsen Frozen Shoulder
DON'T: Make Sudden, Fast, or Reaching Movements
This is the classic aggravator. The inflamed capsule has no "give," so any sudden, unexpected movement will stretch it and cause excruciating pain. Common culprits include:
- Reaching quickly into the back seat of a car
- Trying to catch a falling object
- Reaching for a high shelf
- Reaching behind your back (e.g., fastening a bra, tucking in a shirt). This is often the first and last motion to go
DON'T: Push Into Sharp Pain (The "No Pain, No Gain" Myth)
This bears repeating. This is the worst thing you can do, especially in the "Freezing" stage. Pushing into sharp, 10/10 pain will only increase the inflammation and can make the shoulder stiffer. The golden rule is: "Stretch to discomfort, NOT to pain."
DON'T: Keep It Completely Still (The "Immobilization" Myth)
The flip side of the coin. Many people think, "It hurts, so I should rest it in a sling". This is also wrong. Complete immobilization is what causes secondary frozen shoulder and it will make an existing case much, much worse. You must use gentle, pain-free movements (like pendulum swings) to remind the capsule it's supposed to move.
DON'T: Sleep On Your Affected Side
This puts direct, prolonged pressure on the inflamed joint capsule, aggravating it and guaranteeing you will wake up in pain.
DON'T: Engage in Repetitive Overloading
Even if the movements don't cause sharp pain, repetitive, loading activities can aggravate the chronic inflammation. This includes:
- Repetitive motions at work
- "Overdoing it" at the gym (e.g., trying to push through overhead presses)
- Carrying heavy bags, purses, or groceries on that shoulder
- Slouching at your desk. Poor posture puts your entire shoulder girdle in a compromised position, adding stress to the joint

Unpacking the "Worse at Night" Mystery
This is the most common aggravation of all. As we covered earlier, this happens for two main reasons:
- Mechanical Pressure: Lying down compresses the joint.
- Systemic Inflammation: At rest, your body's inflammatory processes can become more active, and inflammatory chemicals "pool" in the joint, increasing internal pressure and pain.
Other Potential Aggravators
- Uncontrolled Diabetes: High blood glucose can contribute to the glycosylation process that stiffens tissues, likely aggravating the condition's severity.
- Cold: While not clinically proven, many patients report that cold (e.g., cold weather) makes the muscles tense, which worsens the feeling of stiffness.
- Stress: Psychological stress can increase cortisol and systemic inflammation, aggravating the pain.
How long does the freezing stage of frozen shoulder last?
This is a specific question that is almost certainly driven by fear. The "Freezing" stage is the most painful stage. What you are really asking is, "How long will I be in this much pain?"
Defining the "Freezing" Stage (Stage 1)
First, let's be clear on what this stage is. The "Freezing" stage (Stage 1) is the first phase of the condition. It is characterized by:
- The slow, gradual onset of a deep, aching pain
- Pain that gets progressively worse
- A progressive loss of motion as the pain gets worse
- Pain that is typically much worse at night and disrupts sleep
The Timeline: What the Research Says
Direct Answer
Based on clinical data, the "Freezing" stage typically lasts anywhere from 6 weeks to 9 months. This is a frustratingly wide range, but it is the most accurate, science-based answer. It's a slow process.
The Hopeful Distinction: "Freezing" vs. "Frozen"
This is the most critical piece of information and the most hopeful. The severe, constant, night-waking pain is the hallmark of the "Freezing" stage.
The next stage, the "Frozen" stage (Stage 2), is defined differently:
- Pain lessens or subsides
- Stiffness dominates. This is when your shoulder is at its stiffest, but it is often not as acutely painful as the "Freezing" stage
This means you will not be in this severe, 10/10 pain for the entire 1-to-3-year journey. The acute, inflammatory pain will transition into a (less painful) mechanical stiffness problem.
The wide range (6 weeks to 9 months) also suggests that the duration is not a fixed biological timer. It is likely influenced by intervention. An early, effective intervention (like a steroid shot) that "puts out the inflammatory fire" may shorten the duration of this painful stage, not just mask its symptoms.
Your Action Plan for the Freezing Stage
Since this is the stage you're in or asking about, here is your summary action plan:
Goal 1: Pain Control
This is priority #1. Use the strategies covered earlier: NSAIDs, strategic heat/cold, and, most importantly, fix your sleep with the pillow strategies or a recliner.
Goal 2: See Your Doctor
Do not "wait and see". Get an official diagnosis to rule out other problems. This is the stage where a corticosteroid injection can be a game-changer, dramatically reducing the pain and inflammation and potentially shortening this awful phase.
Goal 3: Gentle Motion ONLY
Do not immobilize it. But also, do not start aggressive physiotherapy. This will make it worse. Your only job in this stage is pain-free, gentle motion, like pendulum swings.
Population Focus: How to PREVENT This Stage Entirely
The most powerful information about the "Freezing" stage is how to prevent it from ever happening.
For secondary frozen shoulder, this stage is often 100% preventable. This advice is for the "at-risk" audience: anyone who is about to have (or just had) shoulder, breast, or chest surgery, or has suffered a broken arm, stroke, or rotator cuff injury.
The problem is the immobilization after the event. You must talk to your doctor or physical therapist about early, gentle range-of-motion exercises. Getting the shoulder moving—safely and soon, as directed by your surgeon or therapist—is the single best way to prevent the capsule from ever "freezing" in the first place.