Frozen Shoulder Explained: Causes, Symptoms, and Treatments by Doctors
Dealing with persistent shoulder pain and stiffness can be incredibly frustrating, impacting everything from getting dressed to reaching for something on a high shelf. One common culprit for this debilitating condition is "Frozen Shoulder," medically known as adhesive capsulitis. In this article, we break down what this condition is, why it happens, and what you can do about it, as explained by orthopedic experts.
What Exactly Is a Frozen Shoulder?
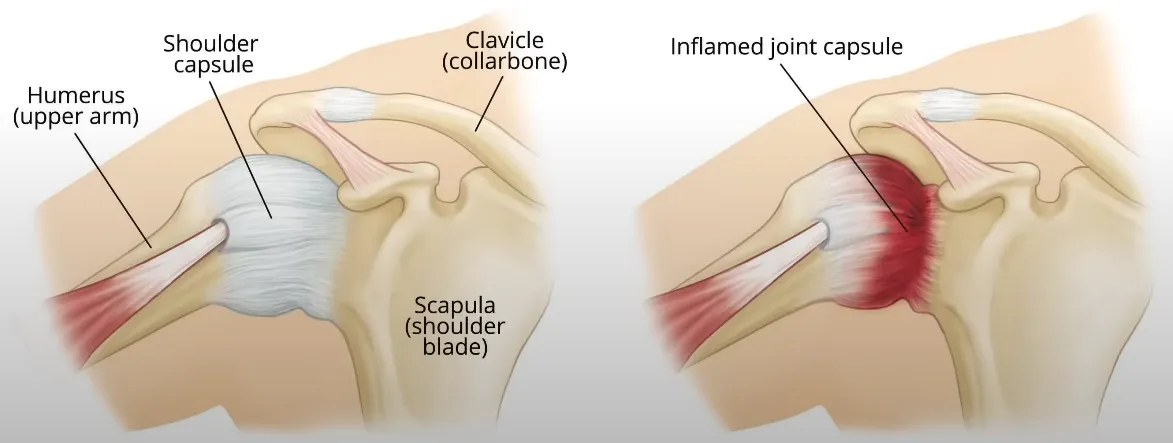
Frozen shoulder, or adhesive capsulitis, is a condition that causes pain and significant loss of motion in the shoulder joint. It occurs when the soft tissue lining that surrounds your shoulder joint, known as the capsule, becomes inflamed, thick, and tight.
The scientific name, adhesive capsulitis, perfectly describes what's happening. "Adhesive" refers to the adhesions or scar tissue that forms, and "capsulitis" means inflammation of the capsule. This inflammation is the root cause of the debilitating symptoms.
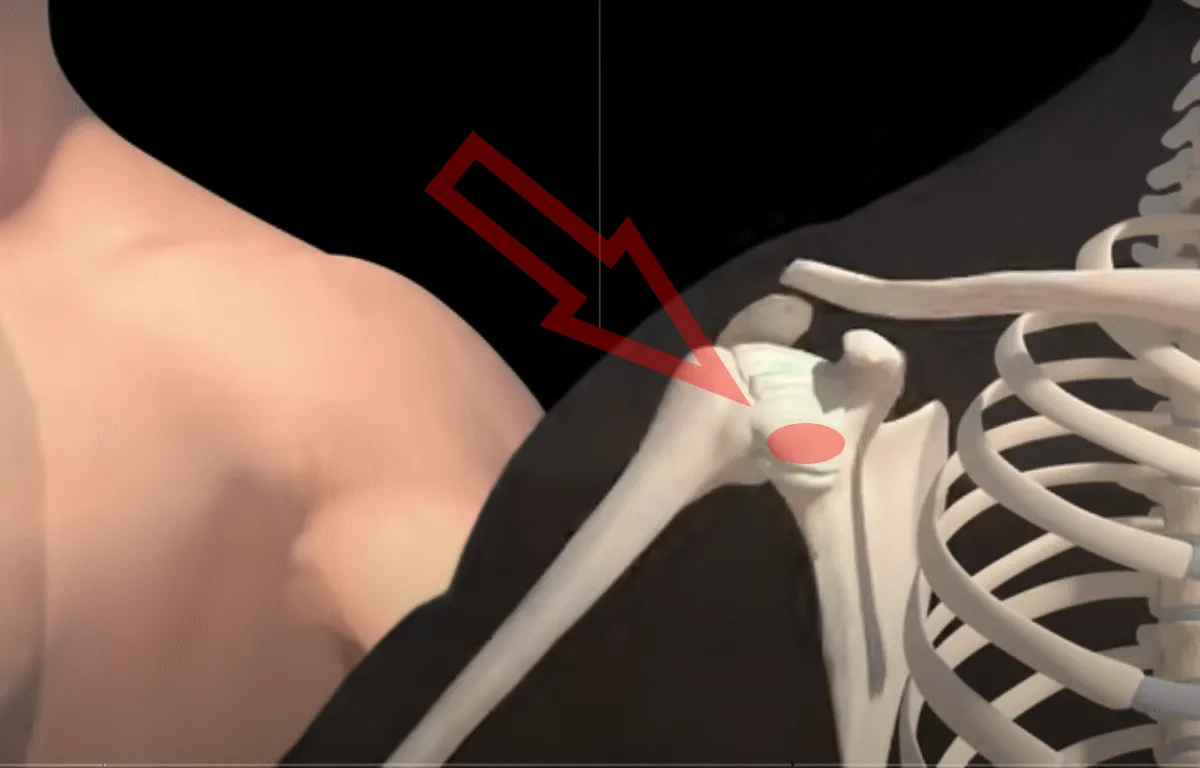
Imagine the lining of your shoulder joint as a thin, supple silk lining that allows for smooth, low-friction movement.
In a frozen shoulder, your body inexplicably changes this lining. It becomes thick, stiff, and more like tough rawhide or leather, severely restricting the joint's ability to move freely.
What Causes Frozen Shoulder?
The transformation of the shoulder capsule can sometimes be triggered by an injury or trauma. However, more commonly, frozen shoulder develops spontaneously, "out of the blue," with no clear cause. This is known as idiopathic frozen shoulder.
Certain factors can increase your risk. The condition is most common in middle-aged individuals, and for reasons not fully understood, it occurs more frequently in women. This may be due to hormonal and structural differences in their shoulder joints, as well as a higher prevalence of risk factors like autoimmune diseases.

Risk Factors for Frozen Shoulder:
- Age 40-60 years
- Female gender
- Previous shoulder injury or surgery
- Diabetes
- Thyroid disorders
- Cardiovascular disease
- Parkinson's disease
If you're experiencing shoulder pain and have risk factors, it's important to understand the complete progression of frozen shoulder symptoms to know what to expect during recovery.
What Does It Look and Feel Like?
The experience of a frozen shoulder typically begins with pain. This pain often appears for no apparent reason and can be quite pronounced at the start.
The pain is usually felt from the top of the shoulder down the side of the arm. As the condition progresses over subsequent weeks, stiffness becomes a more dominant problem. People start noticing they can't perform simple daily tasks, such as washing their hair, reaching for a seatbelt, or getting dressed without significant difficulty and pain.
Common Activities Affected by Frozen Shoulder:
- Washing or brushing hair
- Reaching for a seatbelt
- Getting dressed (especially putting on shirts or jackets)
- Reaching behind your back
- Sleeping on the affected shoulder
- Reaching for objects on high shelves
How Is Frozen Shoulder Diagnosed?
If you suspect you have a frozen shoulder, your doctor will start by taking a detailed medical history and performing a physical examination. During the exam, they will assess your range of motion. A key sign is a limited ability to rotate your arm outward (external rotation) with your elbow at your side. Forward reach and the ability to reach behind your back will also be significantly restricted.
To confirm the diagnosis and rule out other conditions, your doctor will likely order an X-ray. While a frozen shoulder itself isn't visible on an X-ray, the imaging helps to exclude other causes of stiffness and pain, such as arthritis.
Frozen shoulder is a clinical diagnosis, meaning it's primarily identified through your history and physical exam. It generally does not show up on an X-ray or ultrasound. In some cases, an MRI might show the thickened capsule if the radiologist knows what to look for, but it's not typically necessary for diagnosis.
It's important to distinguish frozen shoulder from other issues. For instance, any painful condition, like calcific tendinitis (calcium deposits causing inflammation), can trigger the process of a frozen shoulder. A proper diagnosis ensures you receive the correct treatment.
What Are the Treatment Options?
Thankfully, you're not "frozen for life." There are several treatment options available, though no single one works perfectly for everyone, which is why a multi-faceted approach is often best.
Physiotherapy
One of the first steps is to see a physiotherapist for a stretching program. While therapy alone may not cure the condition, it is crucial for managing pain, improving posture, and gradually regaining motion by working on the surrounding joints and muscles.

A well-designed exercise program using proper rehabilitation tools can be an essential part of your long-term recovery strategy, helping you maintain flexibility as the shoulder capsule gradually loosens over time.
Time and Natural Healing
For most people, the body will eventually heal itself. This process, however, can be long, often taking 12 to 18 months. Over time, the painful phase subsides, and motion gradually returns. Patience is key, as this is often the surest path to recovery.
Injections
Cortisone injections directly into the shoulder joint can be effective for reducing inflammation and pain. Another procedure, called hydrodilation, involves injecting a sterile fluid (saline) into the joint capsule to stretch the tight lining from the inside, much like blowing up a balloon. This can help improve mobility.
What is Hydrodilation?
Hydrodilation is a medical procedure that involves injecting a sterile fluid into the joint capsule to stretch and release the tissues. It's often used as a treatment for frozen shoulder to improve mobility and reduce pain.
Surgery and Manipulation
For persistent cases that don't improve after about 18 months, more invasive options may be considered.
Manipulation under anesthesia is a procedure where a surgeon carefully moves the shoulder through its full range of motion while you are asleep to break up scar tissue.
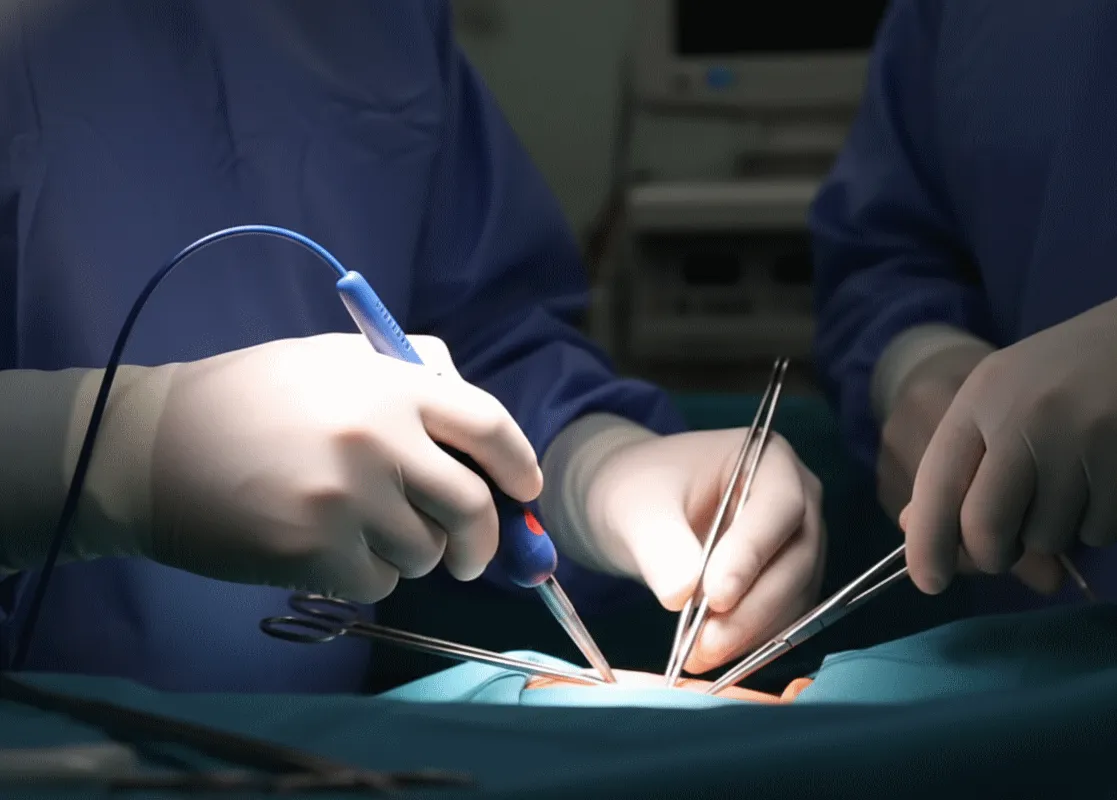
Arthroscopic surgery is another option. Here, a camera is inserted into the joint, allowing the surgeon to see and carefully release the tight capsule tissue. This is often followed by a manipulation to ensure full motion is restored. Immediate, intensive physiotherapy is critical after these procedures to maintain the newfound mobility.
Expert Video Explanation: Frozen Shoulder by Orthopedic Doctors
Watch this comprehensive video explanation from orthopedic specialists who break down everything you need to know about frozen shoulder, from diagnosis to treatment options.
This video provides additional insights from medical professionals about frozen shoulder treatment and recovery.
The Takeaway
Frozen shoulder is a challenging and painful condition, but the good news is that the vast majority of people get better. While it may take time, combining treatments like physiotherapy, medication, and sometimes injections can help manage symptoms and speed up recovery. If you've been suffering for a long time, surgical options can provide relief. Remember to get a proper diagnosis to rule out other issues, and work with your healthcare team to find the best path forward.
Key Takeaways:
- Frozen shoulder (adhesive capsulitis) causes pain and severe motion restriction
- Often develops spontaneously, more common in middle-aged women
- Diagnosis is clinical, based on symptoms and physical examination
- Treatment is multi-faceted: physiotherapy, time, injections, and surgery if needed
- Most people recover fully, though it may take 12-18 months
- Early intervention can shorten recovery time and improve outcomes
For more detailed information on managing frozen shoulder pain and understanding the different stages of recovery, explore our comprehensive pain relief guide which covers instant relief methods, long-term treatment strategies, and specialized care approaches.
Medical Disclaimer
The information provided in this article is for educational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.